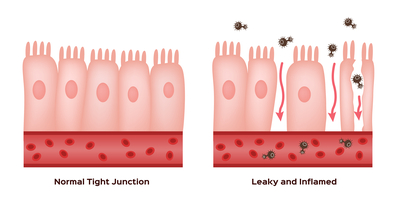
Description
Increased intestinal permeability (leaky gut) of the small intestine can:
- Increase the number of foreign compounds entering the bloodstream
- Allow bacterial antigens capable of cross-reacting with host tissue to enter the bloodstream, leading to auto-immune processes
- Enhance the uptake of toxic compounds that can overwhelm the hepatic detoxification system and lead to an overly sensitized immune system
Leaky gut has been observed in a range of disorders such as:
- Inflammatory Bowel Disease (IBD)
- Food allergy
- Inflammatory joint disease
- Chronic dermatologic conditions
Studies have demonstrated that the increased intestinal permeability observed in patients with ankylosing spondylitis, rheumatoid arthritis, and vasculitis may be an important factor in the pathogenesis of these disorders.
Decreased permeability, on the other hand, appears as a fundamental cause of malabsorption, subsequent malnutrition, and failure to thrive. In certain disease states of the small intestine, such as gluten-sensitive enteropathy, permeability to large molecules may increase while permeability to small molecules decreases – a result of damage to the microvilli. As a result, nutrients become even less available to assist in the detoxification of antigens flooding the system.
Possible causes of increased intestinal permeability (leaky gut) include:
- Intestinal infection
- Ingestion of allergenic foods or toxic chemicals
- Deficient secretory IgA
- Trauma and endotoxemia
- NSAIDs
The Intestinal Permeability Assessment gastrointestinal test directly measures the ability of two non-metabolized sugar molecules to permeate the intestinal mucosa. The patient drinks a premeasured amount of lactulose and mannitol. The degree of intestinal permeability or malabsorption is reflected in the levels of the two sugars recovered in a urine sample collected over the next 6 hours.
test type: urine test